Description
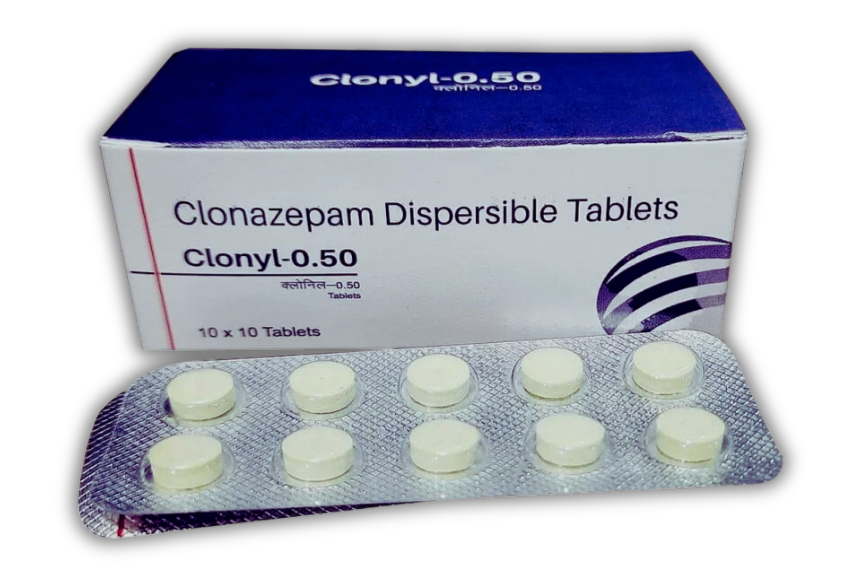
Clonazepam, also known as Klonopin, is a benzodiazepine that needs careful consideration before use. Doctors prescribe it for conditions like epilepsy and panic disorder.
Knowing how clonazepam works, its benefits, and its risks can help you decide if it’s right for you. This isn’t a medicine to take lightly.
In the United Kingdom, clonazepam is a controlled substance under the Misuse of Drugs Act 1971. You can only get it with a valid prescription from a licensed healthcare professional.
You can’t buy clonazepam over the counter or from online pharmacies without proper medical authorisation. Since it affects your central nervous system, the government keeps it strictly regulated and only available under medical supervision.
The cost of clonazepam in the UK depends on the strength and quantity. For example, a pack of 100 tablets at 2mg costs about £71.00, while the same number of 0.5mg tablets is around £44.00.
These prices are for private prescriptions. If you get it through the NHS, you’ll pay the standard NHS prescription charge. Your actual cost may vary based on how you get the medication.
Key Takeaways
- Clonazepam is a prescription-only benzodiazepine mainly used for epilepsy and panic disorder in the UK.
- The drug carries risks of dependency, withdrawal, and side effects, so close medical monitoring is important.
- UK prices for 100 tablets range from £44 to £71 depending on strength.
Clonazepam Clinical Uses and Prescription Status in the UK
Clonazepam is a long-acting benzodiazepine approved for specific conditions in the UK, mostly epilepsy and panic disorder. You need a prescription from a qualified healthcare provider, and the law controls its use due to its dependency risks.
Indications and Approved Uses
Doctors in the UK prescribe clonazepam for epileptic seizures, including absence seizures and other types of epilepsy. It works by boosting the effects of gamma-aminobutyric acid (GABA) in the brain, lowering abnormal electrical activity that causes seizures.
It’s also approved for panic disorder, with or without agoraphobia. Clinical studies show clonazepam helps people with panic attacks, especially for short-term management because of withdrawal and abuse concerns.
Some doctors also use it for muscle spasms and restless legs syndrome. For restless legs, clonazepam can ease those uncomfortable sensations and involuntary movements that mess with sleep and daily life.
Clonazepam Prescription Requirements
You can’t get clonazepam without a prescription from a doctor or qualified prescriber. In the UK, it’s a controlled drug, so prescriptions must follow strict legal requirements.
Prescribers should document the reason for use clearly in your medical records. Sometimes, a consultant gets involved, especially for complex cases.
Specialists in neurology or psychiatry usually start the medication. Sometimes, your GP continues the prescription after the hospital specialist sets up the treatment plan and communicates with them.
Comparisons with Other Benzodiazepines
Clonazepam stands out as a long-acting benzodiazepine, unlike shorter-acting ones like lorazepam or alprazolam. Its longer action keeps blood levels stable and means you don’t have to take it as often.
Compared to diazepam, which is also long-acting, clonazepam is more potent for seizure control. Lower doses of clonazepam can work just as well for epilepsy.
For anxiety and panic disorder, clonazepam offers steady effects without big peaks and drops. The downside is it stays in your system longer, so stopping it takes more time.
Common Off-Label Applications
Doctors sometimes prescribe clonazepam for things it’s not officially approved for. Insomnia is a common off-label use, especially if anxiety or restlessness keeps you up at night.
Some clinicians try it for generalised anxiety disorder, though that’s not a licensed use in the UK. It’s also considered for akathisia in psychiatric settings.
In status epilepticus, a serious type of seizure, clonazepam might be used, though lorazepam or diazepam are usually preferred first. Off-label use always needs good documentation and regular reviews to keep things safe.
Mechanism of Action, Efficacy, and Dosing
Clonazepam increases GABA activity in your brain, which calms things down and helps with seizures and anxiety. Its effectiveness is proven for several conditions, but the right dose depends on your needs and diagnosis.
How Clonazepam Works in the Body
This medication acts as a CNS depressant. When you take clonazepam, it binds to GABA-A receptors in your brain.
GABA is the main inhibitory chemical messenger in your brain. Clonazepam boosts GABA’s effect, making nerve cells less excitable by opening chloride channels more often.
It also increases serotonin synthesis, which helps explain its effect on both seizures and some psychiatric conditions. As a 7-nitrobenzodiazepine, clonazepam’s effects come on at a moderate pace but last longer than shorter-acting benzos like lorazepam or alprazolam.
Efficacy for Mental Health and Neurological Disorders
Clonazepam works well for panic disorders and different types of seizures, including absence and myoclonic seizures. Randomised controlled trials back up its use both alone and with other medicines.
For panic disorder, studies show people generally improve. The medication can help with severe anxiety if other treatments don’t work.
In acute mania, clonazepam can quickly calm symptoms, often alongside mood stabilisers or antipsychotics. Still, benzodiazepines are best kept for short-term use in those cases.
Some off-label uses—like restless legs syndrome, tardive dyskinesia, and agitation in acute psychosis—have also shown benefits.
Typical Dosage and Administration
Your starting dose depends on your condition. For seizures, adults usually start at 0.5 mg three times a day, gradually increasing up to a max of 20 mg per day split into several doses.
For panic disorder, treatment often begins at 0.25 mg twice daily. Your doctor might bump this up to 1 mg per day after a few days, and some people need up to 4 mg daily for full effect.
Key dosing tips:
- Take doses evenly spaced throughout the day.
- Increase slowly to avoid too much sedation or side effects.
- Never stop suddenly; withdrawal can be dangerous.
- Elderly patients need lower doses—they’re more sensitive to the effects.
Therapeutic Comparisons: Systematic Reviews and Meta-Analyses
Meta-analyses show clonazepam’s long duration gives it an edge over shorter-acting benzos like alprazolam. You get steadier blood levels, which can mean fewer breakthrough symptoms.
Systematic reviews for panic disorder find clonazepam works as well as other benzodiazepines but doesn’t need to be taken as often. It’s more potent than diazepam, so lower doses do the trick.
Compared to antidepressants for anxiety, benzodiazepines like clonazepam act faster but carry more dependency risk. They’re best for short-term use while other treatments kick in. In epilepsy, clonazepam works well as an add-on, though some people develop tolerance over time.
Adverse Effects, Long-Term Safety, and Dependency
Clonazepam can cause anything from mild drowsiness to serious dependency problems. Being aware of both short-term side effects and long-term risks helps you make better choices.
Common and Serious Side Effects
Most people notice drowsiness, fatigue, or dizziness when they start clonazepam or after a dose increase. Impaired coordination and sleepiness can make driving or using machinery risky.
Headaches and low mood sometimes show up, especially if you already have depression. It’s not a medicine to take before an important meeting, that’s for sure.
Common Side Effects:
- Drowsiness and sedation
- Fatigue and weakness
- Dizziness and unsteadiness
- Impaired coordination
- Difficulty concentrating
Serious side effects need urgent medical help. These include severe confusion, hallucinations, or big changes in mood or behaviour. Some people get paradoxical reactions—more anxiety or agitation instead of less.
Long-Term Effects and Tolerance
Using clonazepam for a long time leads to tolerance. You may need higher doses for the same effect as your body adapts.
Long-term use can chip away at your focus and motivation. Work and relationships might suffer. Older adults especially face higher risks like cognitive impairment, delirium, and falls.
Physical dependency can develop even if you stick to the prescribed dose. Research on deprescribing in older people shows that with the right support, many can reduce or stop clonazepam, but it takes careful monitoring.
Memory and mental sharpness often get worse with long-term use. Unfortunately, these effects sometimes stick around even after stopping the medication.
Risks of Addiction, Withdrawal, and Overdose
Clonazepam carries real risks of addiction and misuse. Physical dependence can set in after just a few weeks, making it tough to stop without help.
If you reduce or stop clonazepam suddenly, withdrawal symptoms can appear—seizures, tremors, sweating, confusion, and anxiety. The risk of seizures is especially serious.
Withdrawal Symptoms:
- Seizures (most dangerous)
- Tremors and muscle pain
- Excessive sweating
- Confusion and hallucinations
- Rebound anxiety and insomnia
- Nausea and vomiting
Overdosing on clonazepam can cause breathing problems, extreme drowsiness, and loss of consciousness. Mixing it with alcohol, opioids, or sleeping pills makes overdose much more likely. Flumazenil can reverse an overdose in emergencies, but it has to be used carefully since it can trigger seizures.
Managing Adverse Effects and Dependency
If side effects bother you, talk to your prescriber before making changes. Some side effects fade after a few weeks as your body gets used to the medicine.
To reduce dependency, doctors recommend tapering the dose slowly under supervision. Cutting the dose by 25% every two weeks, along with sleep advice, helps many people come off clonazepam. This usually takes about five appointments over several weeks.
For those struggling with misuse, addiction treatment programmes offer medical and psychological support. Your GP can refer you to specialist services if needed.
Never stop clonazepam abruptly. A slow, supervised reduction helps your nervous system adjust and keeps withdrawal risks lower. Regular checks of blood pressure and other vital signs help catch problems early during the process.
Clonazepam Availability, Cost, and Patient Guidance in the UK
Clonazepam needs a prescription in the UK. You can get it from NHS or private pharmacies, but prices can vary quite a bit.
The NHS has put out updated safety advice for anyone taking this benzodiazepine. They stress the importance of regular monitoring and using it properly.
UK Clonazepam Cost Overview
You can’t get clonazepam in the UK without a prescription from a registered medical professional. It’s strictly prescription-only, no way around that.
Private pharmacy prices shift depending on the dose and how many tablets you need. Based on UK-Pharm24’s data, a 30-tablet pack of 2mg clonazepam is about £89.00.
If you need 60 tablets, that’s around £129.00. A 90-tablet supply goes for roughly £179.00, and 180 tablets can reach £319.00.
NHS prescription costs are a flat fee per item. If you qualify for free prescriptions or have a prepayment certificate, you won’t pay the standard charge.
Brand choice can impact both price and supply. The NHS suggests sticking with the same brand if possible, but your doctor will help decide what’s best for you, especially if seizure control is tricky or your treatment history is complicated.
Patient Advice on Safe Use
Clonazepam boosts gamma-aminobutyric acid (GABA) in your brain. This chemical calms nerve activity, helping with seizures, muscle spasms, and panic symptoms.
Don’t just stop taking clonazepam out of the blue. The NHS says you should always reduce the dose slowly—especially if you have epilepsy—since stopping suddenly can cause withdrawal or even trigger seizures.
Keep your medication somewhere safe and only take it exactly as your doctor tells you. Stick to the timing and dose instructions as closely as possible.
If you miss a dose, check your patient leaflet or call your prescriber. It’s better to ask than guess.
Let your healthcare provider know if you notice anything weird—like extra drowsiness, mood swings, or trouble breathing. Those regular check-ups really do help keep things on track.
Key Considerations for Benzodiazepine Therapy
NICE and NHS both highlight the need for careful prescribing with benzodiazepines like clonazepam. Your doctor should keep reviewing your treatment to see if it’s still needed and working well.
Long-term use can lead to dependence or addiction, so your healthcare team should talk with you about how long you’ll take it and the risks. Sometimes, they’ll suggest other treatments instead.
Watch out for drug interactions. Clonazepam gets broken down by the liver enzyme CYP3A4, so other medications can mess with its levels in your body. Always tell your doctor about everything you’re taking, even supplements.
Some health conditions mean clonazepam isn’t safe for you. Your doctor will go through your medical history before prescribing and might need to adjust your dose based on your situation.
Frequently Asked Questions
People have a lot of questions about clonazepam—how it’s used, how safe it is, how fast it works, dosing, different tablets, and the rules around it in the UK.
What are the main clinical uses of clonazepam in the UK, and how does its effectiveness compare across approved and off-label indications?
In the UK, clonazepam is licensed for treating epileptic seizures, panic disorder, and involuntary muscle spasms. It’s especially good for certain seizure types like Lennox-Gastaut syndrome, myoclonic seizures, and absence seizures.
For panic disorder, clonazepam often helps lower both the number and intensity of panic attacks. Many people notice a difference within the first couple of weeks. Some doctors also prescribe it off-label for restless legs syndrome, though that’s less common.
Clonazepam usually provides reliable seizure control as part of an epilepsy plan, but your results can vary. Some people find it works better than other benzodiazepines for certain seizure problems.
Off-label uses include things like acute mania, sleep disorders, and some movement disorders. The evidence for these is thinner, so your doctor will weigh the risks and benefits carefully before prescribing for those reasons.
What are the most common and most serious side effects of clonazepam, and which warning signs should prompt urgent medical advice?
The most common side effects are drowsiness, dizziness, and problems with coordination. These usually show up early on and might fade as you get used to the medication.
Fatigue and trouble concentrating are also pretty common. Higher doses can cause memory issues or confusion, and you might notice slurred speech or feel off-balance.
Some people experience depression or mood changes, so keep an eye out for those. If you get any of these, tell your doctor.
Serious side effects need immediate attention. If you have a severe allergic reaction, trouble breathing, or chest pain, get help right away.
If you start having suicidal thoughts or your depression gets much worse, seek professional help immediately. Sometimes, clonazepam can actually cause more anxiety, agitation, or aggression—especially in kids or older adults. If this happens, stop taking it and call your doctor right away.
Respiratory depression is a real danger, especially if you mix clonazepam with alcohol or opioids. Watch out for very slow or shallow breathing and extreme sleepiness. Any big changes or worsening in your seizure pattern also mean you should get medical help fast.
How long does clonazepam typically take to start working, how long do its effects last, and what factors can change its duration of action?
For panic disorder or restless legs syndrome, clonazepam usually starts working within about an hour. Some people feel calmer pretty quickly. The medication hits peak levels in your blood between one and four hours after you take it.
For seizures or muscle spasms, it might take a few days to a week to see the full effect. That’s because your doctor will slowly increase your dose to find what works best for you.
Generally, a single dose lasts about six to twelve hours. That’s why it’s often taken two or three times a day. Some folks process the drug more slowly and feel the effects for longer.
Your age makes a difference—older adults usually break down clonazepam more slowly, so the effects last longer. Liver function matters too; if your liver doesn’t work as well, the drug sticks around in your system longer.
Taking clonazepam with food might slow absorption a bit, but it doesn’t really change how well it works. Other meds can speed up or slow down how your body handles clonazepam, and if you smoke, your body might clear it out faster.
What is the recommended dosing range for clonazepam in adults, and what is considered the maximum safe total dose within 24 hours?
For seizure disorders, adults usually start at 1 mg per day, split into smaller doses. This helps your doctor see how you handle the medication.
Panic disorder treatment typically starts at 0.5 mg twice a day. Starting low helps avoid too much sedation or side effects, and your doctor will adjust based on how you respond.
Maintenance doses for epilepsy are often between 4 mg and 8 mg daily, divided into several doses. Some people need less, others a bit more, depending on their needs.
The highest recommended dose for adults with seizures is usually 20 mg per day. For panic disorder, the max is generally 4 mg daily. Going over these limits raises the risk of serious side effects without extra benefits.
If you’re over 65, you’ll probably need a lower dose since your body processes the medicine more slowly. Doctors usually start older adults at half the typical adult dose and increase it more cautiously.
How do different tablet strengths (such as 0.5 mg and 1 mg) affect dosing strategies, titration, and risk of dependence or withdrawal?
Lower strength tablets, like 0.5 mg, make dose adjustments easier during titration. Your doctor can bump your dose up in smaller steps, which usually means fewer side effects.
This gradual process helps you and your doctor figure out the dose that actually works best for you. Sometimes it feels like trial and error, but it’s worth it.
Higher strength tablets, such as 1 mg or even 2 mg, are more convenient for folks on steady, higher doses. Taking fewer pills just makes life simpler for a lot of people.
But with those larger strengths, you lose some flexibility if you need to lower your dose. That can be a pain if you ever need to cut back.
Total daily dose matters more for dependence risk than the strength of each tablet. You can still develop physical dependence whether you take several small tablets or just one big one.
Honestly, it’s the length of time you use the medication that really shapes dependence, not just the size of each pill.
Tapering off gets a lot easier if you have lower strength tablets available. Dropping by 0.5 mg at a time is less harsh than making bigger cuts.
Your pharmacist can mix and match different strengths to help you step down your dose more gently. That sort of flexibility can make a huge difference.
The 0.5 mg tablets are especially handy during withdrawal. You can set up a tapering plan that lets you cut back slowly, sometimes over weeks or even months.
Stopping suddenly, no matter the strength, is risky. Withdrawal seizures and other nasty symptoms are a real threat if you quit cold turkey.